A recent survey conducted by #MEAction UK found that UK specialist myalgic encephalomyelitis (ME) services are not fit for purpose. Areas investigated included:
- Management strategies
- Experience attending a clinic
- Cognitive behavioural therapy (CBT)
- Activity management
The survey was conducted to provide evidence to the National Institute for Health and Care Excellence (NICE) in response to their latest call for evidence. #MEAction UK has submitted the survey report along with a range of studies and surveys relevant to this call. NICE are re-writing their guidelines on ME, with new guidelines due to be published in October 2020.
The survey was conducted online, with the questionnaire available between 24th September and 7th October, 2019. An online methodology was used in order to meet the deadline for evidence set by NICE: time constraints did not allow for paper based surveys to be sent out. A total of 1,906 respondents completed the survey by the deadline.
[maxbutton id=”23″ url=”http://www.meaction.net/wp-content/uploads/2019/10/MEAction-submission-to-the-NICE-ME-CFS-call-for-evidence-consultation.pdf” text=”Read the full submission” ]
#MEAction UK identified the potential for patient data to enhance NICE’s guideline development. Considering there is a lack of evidence in specific areas identified by NICE, we felt it was imperative to provide further evidence – working to create a balance between the professional judgement being used to write these guidelines and the expertise by experience of people with ME especially where the wisdom of these two evidence sources contradicts.
With regards to management strategies during assessment for diagnosis, results showed that healthcare professionals are commonly providing advice to maintain or increase activity during this period. Almost 9 out of 10 respondents deteriorated having followed this advice, compared to less than 1 in 10 who were told to rest. Healthcare professional’s initial advice had a significant effect on patient outcomes:
- 23.9% of respondents were told to increase their activity levels. 90% of these respondents reported that they deteriorated having followed this advice
- By comparison, of the 21.6% of respondents who had been told to decrease their activity and rest, 36.8% improved and only 9% had deteriorated
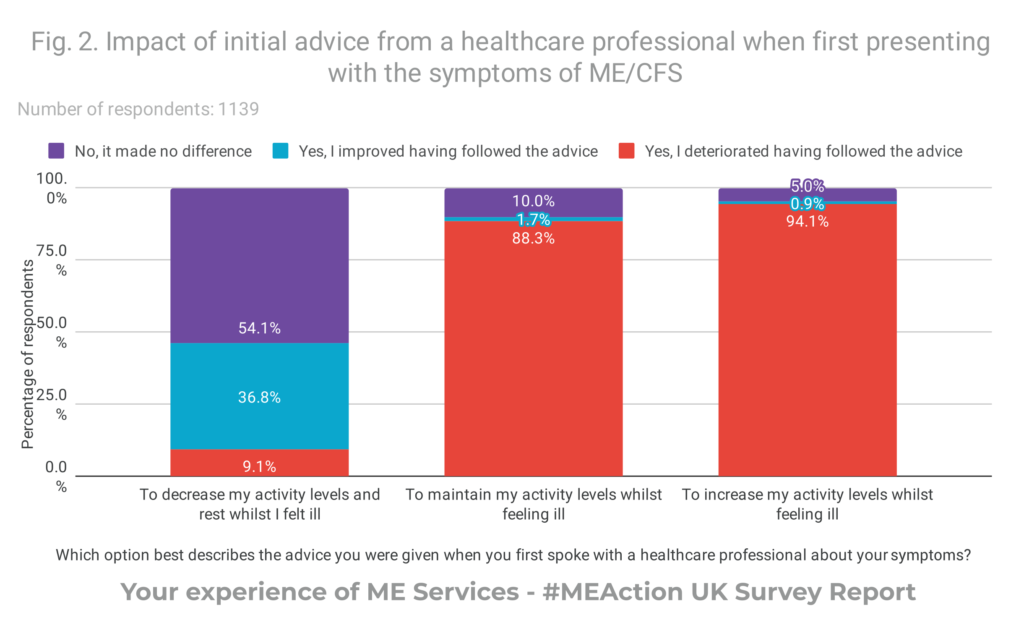
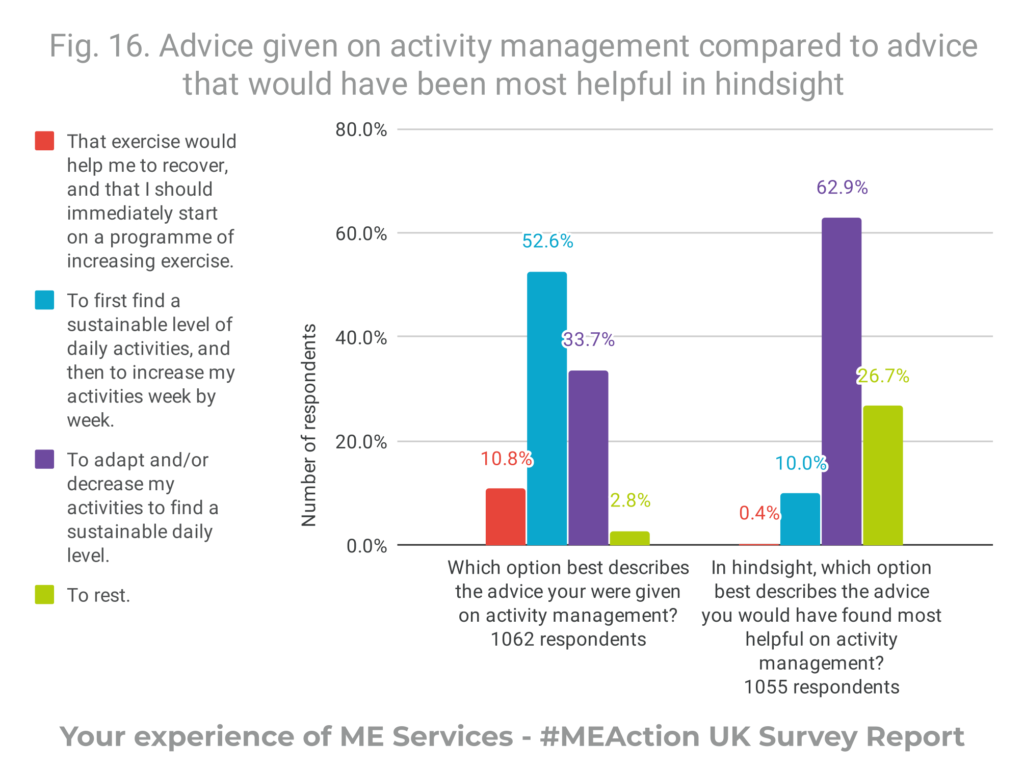
94.4% of respondents reported that, in hindsight, the most helpful advice they could have been given when first presenting with symptoms of ME was to decrease activities and rest whilst ill.
In relation to methods of monitoring and/or reviewing, results identified that there was a failure of services to provide ongoing support or follow up and this left respondents feeling abandoned and without help. Furthermore, respondents thought that services should be led by a consultant, with support from professionals trained in the causes and impact of ME.
With respect to people’s experience of interventions for ME, respondents reported that many ME services are providing unsuitable advice and treatments that often have a negative impact on patients’ health. Moreover:
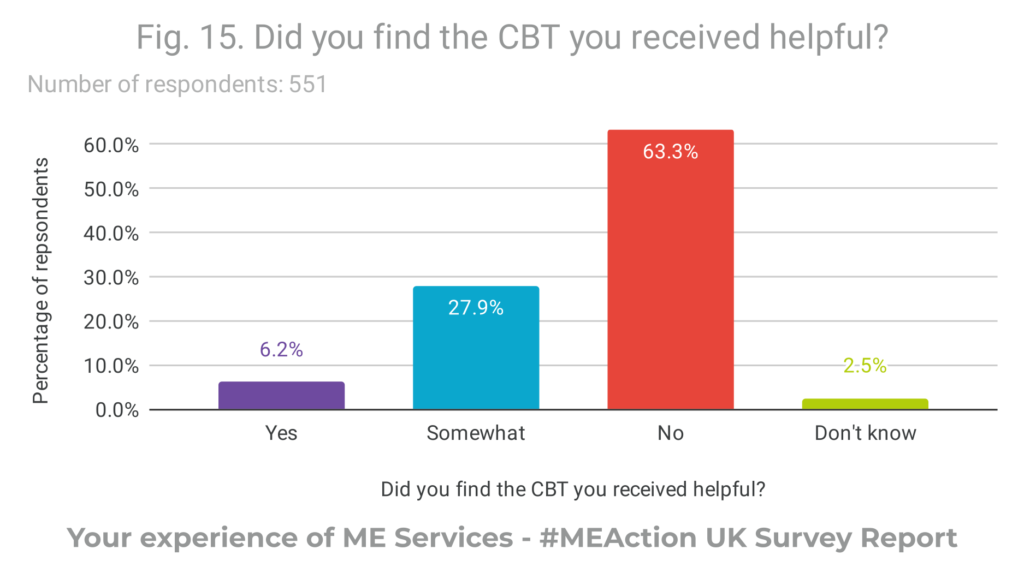
- CBT was not helpful to a majority of respondents
- Advice received on activity management and increasing activity was contrary to what respondents reported would have been most helpful in hindsight
- Respondents were commonly pressured to undergo treatments
- Overall, respondents wanted current services either to adapt or to be entirely rebuilt with patient input, confirming that current services are failing to meet the needs of patients
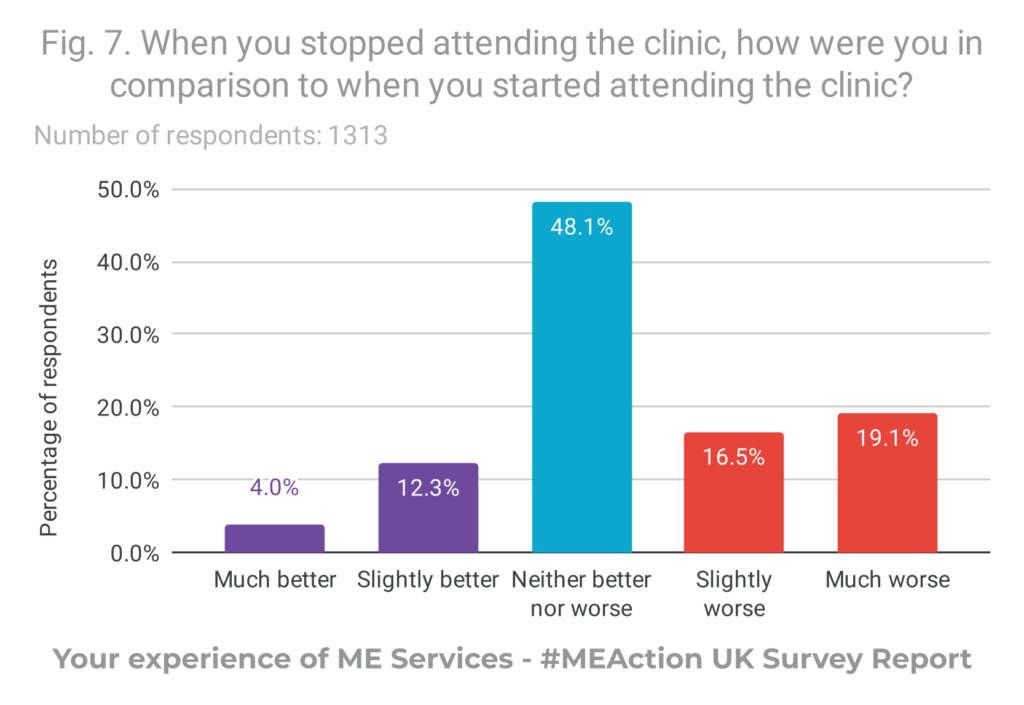
- Almost half of respondents said they were neither better nor worse (48.1%) after attending an ME service. Of the 51.9% of respondents who reported that attending the clinic changed their health status, over twice as many reported they were worse having attended the clinic than reported improvement.
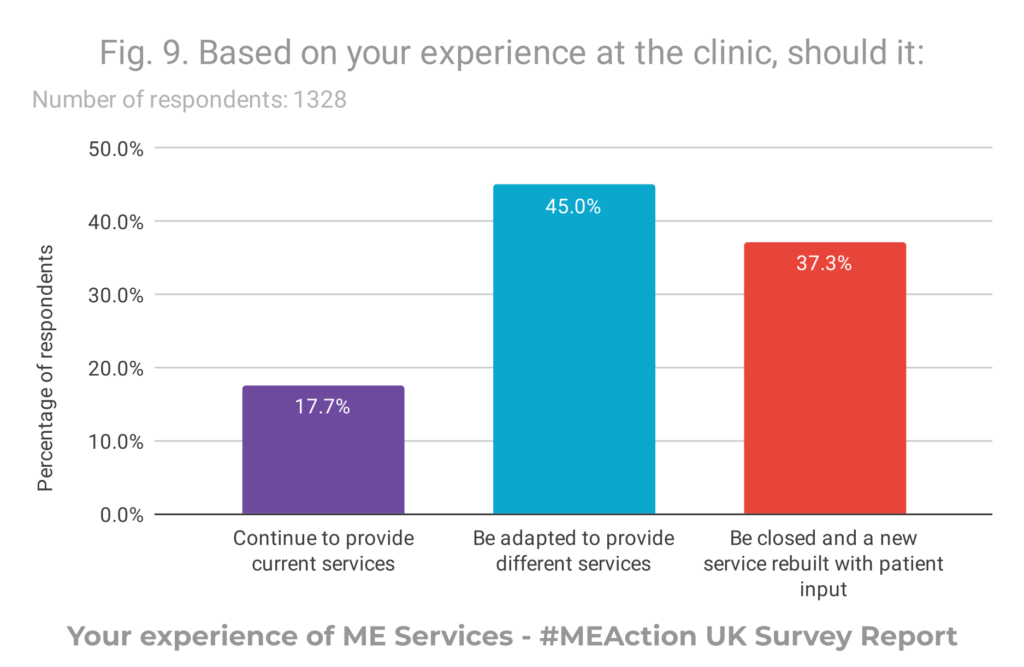
#MEAction UK concluded that current ME services in the UK are not fit for purpose and urgent change is required.
Check out these charts explaining the responses in more depth, or read the full report with breakdowns of impact and experience by clinic attended:







3 thoughts on “ME Services in the UK Not Fit for Purpose”
In my 2012 book, ‘A Beginner’s Guide to ME/CFS’, which is basically a manual on the importance of rest, how to minimise exertion, being grateful to carers who offer physical help, I wondered whether: ‘Exercise Will Make You Worse, More Exercise Will Make You Much Worse, and Even More Exercise Can Have You Incapacitated and In Pain for The Next 20 Years’ was too extreme.
It is wonderful to know that it was not…that the advice I gave will have helped those who followed it.
Why? In light of these findings, cannot NICE suspend the current detrimental and downright dangerous and hideously outdated, so called guidelines. Whilst the retraining of Occupational therapists and the medical profession is actioned, act on the side of common sense and actively encourage rest and meditation.
They could also recommend that more effective assistance is provided with the employment of domestic carers to reduce the strain on ME/CFS Fybromyalgia afflicted patients and their immediate carers, predominantly close family.
A really impressive and valuable report. Thanks to all who worked on it and got it completed/submitted in such a short space of time.
Comments are closed.